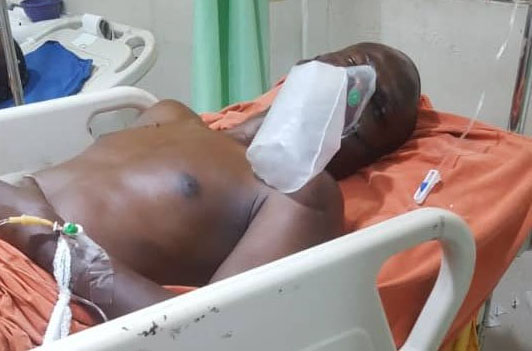
Ibrahim Sule, a former correspondent with THISDAY, lost his life while on admission at the accident and emergency ward of the Lagos University Teaching Hospital (LUTH) on September 3, 2017.
Some of the people who were with him in his dying hours said but for the negligence of staff of the hospital, Sule would have been alive.
In a petition to the chairman of the medical advisory committee of LUTH, Cornelius Ojo, an independent consultant, asked the hospital to take responsibility for the tragic incident.
Ojo, a long-time friend of the deceased narrated how he called the attention of health workers to the plight of Sule when he was struggling for his life but adequate steps were not taken to save him.
Advertisement
He said while nurses preferred to chat and surf the internet while on duty, doctors were missing during emergency.
Below is his petition:
Ibrahim Kayode Sule, a former Senior Correspondent with Thisday newspapers and a media consultant until his tragic death, is a long-time friend of 25 years. He was both a classmate and a course mate at the department of mass communication, University of Lagos. Since we graduated 20 years ago, we remained glued until death separated us on Tuesday 3rd September 2019, while under the negligent care of staff of Ward A2, Lagos University Teaching Hospital (LUTH), Idi-Araba, Lagos.
Advertisement
We had both been invited to Ileya/Ojude-Oba 2019 by another mutual friend. In fact, I passed the night of Saturday 10th August 2019, at his 3-bedroom flat, Iponri Estate, Off Bode Thomas in Surulere. We left for Ijebu-Ode early Ileya morning on Sunday 11th August, 2019, and returned to Lagos on Tuesday, 13th, August, 2019. That was the last time I saw him. He was aware of my trip outside Lagos on 22nd of August, 2019. I returned to Lagos on Thursday 29th August 2019, and a call was placed to him at 2130hrs to inform him I was back in Lagos, but no response. I had thought he was busy and would call back. I was wrong. The following morning 30th August, 2019, I received a call from his neighbour, asking me to come over to LUTH. I arrived LUTH’s A&E shortly after, and met him in bed still in coma, and with the aid of oxygen.
The above brief note is to avail the Management of my closeness to him, and which necessitated my close watch on him while under the care of LUTH. I present below, sequence of events leading up to his avoidable death.
WHILE AT THE A & E
My observation at the A&E was that of a man still in coma and being sustained by oxygen. As I went in and out, I later discovered an open sore in his left hind leg with body fluid streaming onto the stretcher. I was upset that his wound, apparently from his unexplained domestic accident was left undressed three days after his admission. I thought it was against infection control to leave a wound undressed. What about Tetanus risk to the patient? As many questions agitated my mind, I turned to go and lodge a complaint. I then saw one of the A&E doctors passing by, and I approached him. Without allowing me to explain my concern, he quickly pointed at the nurses (meaning – “talk to them”). I went over to the nurses and beckoned to one of them to please come. I expressed my displeasure to her that his wound was left undressed, and I showed him the body fluid and tiny whitish flies around the wound areas. She suggested it was a bed sore and that they were going to dress it. I countered that it couldn’t have been a bedsore, being not a bony area where a bedsore could occur (hind leg) quickly. I also suggested to her that anti-tetanus would be needed to prevent another medical issue. Thereafter, the sore was dressed and I was informed later that anti-tetanus was prescribed, bought and administered. It should be noted here that, those actions were taken only after my observations and complaints. I left the hospital at about 10pm that Friday, but another friend was detailed to stay behind for the night.
Advertisement
I returned the following day Saturday 31st August, and I was informed by the colleague who stayed overnight that he became conscious in the morning and asked few questions like “where is my mobile phone”?; “Where are we”? etc. A nurse later corroborated this and added that he was asked to lift his leg and arm and he responded. I was eager to witness that scenario again, but unfortunately he remained unconscious for the rest of the day. I left around 11pm that night. On Sunday 1st September, I arrived early. Fortunately, I went in at a time he was awake – his eyes were wide opened and I greeted him and asked if he could recognise me. He stared at me and blinked normally, with an attempt to turn his head. He also slightly raised his left arm and used same to scratch his stomach. Unfortunately, he couldn’t utter a word before slipping into coma. He never opened his eyes again till he tragically passed away.
FAMILY MEMBERS DENIED ACCESS TO HIM
Later that Sunday afternoon, we were informed he would be transferred to the ward. Personally, I didn’t think he had recovered and stabled to be transferred from the A&E care. But who am I to object? When it was time to move him later in the night to Ward A2, I witnessed another odd spectacle that was inimical to a patient in coma. We were called to come and join the only staff assigned to move him. I knew it was unprofessional and risky to ask family members not trained in ‘patient handling’ to move a patient in coma from the bed to a stretcher, without moving/handling equipment. I then asked the staff if there was a sling – a sheet that aids moving a patient without pushing/shoving the patient. “Not available”. I was told. So oddly, about 4 of us moved him from the bed to the stretcher. It was obvious he was in distress as we moved him (he groaned). The same crude method was used to transfer him to bed when we arrived at Ward A2. Meanwhile, his eyes remained closed. Before we left late that Sunday night, we bought another oxygen gas as a back-up to the one just fixed. It is worth stating here that, we were told no one could stay behind in accordance with the “ward Policy”, but that someone should come as early as 5.30am to come and do personal care for him. I found this arrangement shocking and against Standard Operating Procedure (SOP) – family members being asked to carry out personal care for patients on admission. We had no choice than to detail someone to make the early morning trip to do the personal care.
When I arrived on Monday, the fellow who came early in the morning informed me that he remained asleep, and that the oxygen mask was removed for few hours because nurses said his breathing “improved”. Whether the removal of the oxygen for those few hours was on a doctor’s instruction, I couldn’t tell. But when I went in to check on him, his breathing had changed compared to the situation at the A&E. The breathing was more of a struggle and thick sputum (my guess) was coming out of his mouth. I was concerned, but a nurse told me it was an effect of oxygen use and that they were cleaning him intermittently. Throughout that Monday 2nd September, he remained “asleep”. Again, before we left that night, we asked if they would be needing anything, we were told to make a back-up oxygen available. We did before leaving.
Advertisement
OXYGEN NOT WORKING
On Tuesday 3rd September, I arrived at about 11am and I met about 7 other friends and family members who already arrived before me. A colleague detailed to come early 5.30am told me he already carried out personal care on him. But thereafter, no one was allowed-in again as they were conducting “examinations”. Of course we could see as many people as possible inside the ward (I guess they were medical students and their lecturers). When I made enquiries from the security man at the locked gate to the Ward, he told me no one would be allowed-in until after the examinations which he said would end at 3pm or thereabouts. By 1410hrs, I was no longer comfortable not seeing him since morning. I quickly approached a nurse who dashed out and was dashing into the Ward. I told her I just wanted to go in to have a quick check on him. After much argument, she allowed me in and said I should make it “brief”. Getting to his bedside, I discovered his breathing had changed to a distressed one. I moved closer and discovered the oxygen was not working – the humidifier bottle was in a ‘sleep’ mode and the reservoir bag was also not functioning properly as when the oxygen is working. With the oxygen not working and the mask still covering his nostrils, it was obvious that his breathing was jeopardised. How on earth did they not notice this bad situation? I called a senior nurse’s attention and she said the oxygen wasn’t exhausted yet, that it was the “water in the humidifier bottle that was finished”. She then added water in my presence and I could see the bottle in action.
Advertisement
The question that agitated my mind was: how long had the water in the humidifier bottle finished without being topped up? So, if I did not go in, they did not notice it had stopped. Not satisfied, I checked the oxygen gauge and I discovered it was close to 0 point. I called her attention to it, but she quickly dismissed it that they “don’t” rely on the gauge as it usually malfunctions. It’s the humidifier bottle that “let us know if the oxygen is finished”. She told me. Not satisfied, I used my mobile phone to snap the oxygen cylinder gauge and left the ward in anger. At about past 1600hrs, I went in again and discovered the same problem – oxygen wasn’t working and the humidifier bottle was also in a non-functional state. Yet, the oxygen mask was on him (making his breathing more difficult). I then checked the gauge and discovered it was on zero. I called the nurse again to come (the nurse on duty when I complained earlier had left). Another set of nurses had taken over – 3 of them). When she looked and saw I was right, she then panicked and asked us to “go buy another oxygen quickly”. As I detailed two other guys with me in the Ward to go for the oxygen, I stayed behind and I asked her whether it was the duty of family members to be carrying out their job of checking the oxygen; after all, you prevented us from coming-in since morning. I informed her I had envisaged trouble earlier on before the other nurses left and I wondered why 3 of them sitting so close to his bed could not notice that he was in distress and that the oxygen was exhausted. This time, I could not keep the negligence to myself. I went outside the Ward to lodge a complaint. It is worth stating here that the processes involved in buying oxygen could take an hour and more depending on how long the queues are at various points.
DOCTORS MISSING IN ACTION
Advertisement
I called SERVICOM on mobile No 08183983778 at about 1638rs to report NEGLIGENCE by nurses and we spoke for 4 minutes and 27 seconds . The female voice on the SERVICOM number while admitting it was the duty of the nurses to monitor the oxygen, tried to suggest that they were probably busy. But I insisted to her that, they couldn’t have been so busy as to neglect a patient whose lifeline was the oxygen. I told her they were all seated at the time I went inside, and the patent’s bed was so close to them that it was easy to know if the humidifier bottle was working or silent. She then directed that I should return to the Ward and make my complaints known to the Matron. The conversation barely ended when one of the nurses – a male rushed outside and asked me to “get the people who went to buy the oxygen to hurry up” With that statement, I knew the situation was dire. I rushed in with him and met other nurses trying to revive him by pumping his chest. I moved closer, held his left hand and it was so cold – I knew it was a bad situation. They were calling many doctors for the next 20 minutes, but sadly there was no emergency doctor within LUTH to come and help. Ibrahim Kayode Sule was dead. I knew they were beating a dead horse with the resuscitation drama. He was dead. At this time other family members were noticing the situation, but I asked them to stay outside and allow the nurses to do their job. This was to prevent an ugly situation as it was apparent to everyone that he was neglected by those who prevented us from checking on him since morning because of the “examinations” being conducted.
With the battle lost, I went quickly to the Police Post to lodge a complaint of CRIMINAL NEGLIGENCE leading to a loss of life. The Police called the LUTH’s Chief Security Officer (CSO) who spoke to me briefly and asked me to wait for him at the Police Post. To keep managing the situation from degenerating, I dashed back to the Ward to keep everyone at bay, telling them a doctor was being awaited and that he had been “revived”. Meanwhile, the nurses had covered him up having realised their drama was of no effect. By this time, the oxygen had arrived, but my friend was gone. The Police called me on phone to return to the Police Post where the CSO was already waiting for me. I narrated the sequence of events to him and he put a call across to the head of SERVICOM and they discussed. He then detailed 2 Policemen to follow me to the Ward, where a female doctor was already there to certify the patient dead. The said doctor was trying to narrate the situation to me and how the nurses “tried their best” to save the situation, but which unfortunately did not work. I thanked her and made it clear to her that I witnessed the soul-destroying events leading to his death and that it was plain NEGLIGENCE. The nurses were only trying to cover-up their negligence by resuscitating a dead person. I insisted to the doctor.
Advertisement
To begin with, I did not think that my friend should have been transferred out of the A&E at the time he was moved. The surveillance level on the patients at the A&E was high compared to the lukewarm attitude at the ward level. Aside those two occasions of sub-consciousness as explained above, there was nothing more to suggest his condition was fit enough for a transfer. He was not fully back into consciousness. And in any case, if he was deemed medically fit enough to be transferred to the ward, he should have been placed on between 15 – 30 minutes observation and not on general observation. It was mind-boggling that a patient whose sustenance depended solely on oxygen could be left unattended to, till the oxygen ran out without detection.
As chronicled above, my observations generally is that the level of care at LUTH was low and staff attitude to their work, particularly the ‘duty of care’ they owe the patients was partially on display and not encouraging. The shabby treatment being meted to family members who were trying to safeguard their loved ones was another humiliating scenario I noticed. The use of phone at work and while attending to clients also call for concern. It is generally disrespectful for anyone at work to be making private calls, face-booking or chatting while purporting to be busy at the same time. Some staff could be seen with the earpiece on, in a rare display of gross indiscipline by staff of a leading teaching hospital. There is a compelling need for the Management to rise to the occasion and save the reputation of LUTH from total collapse. The time for a turnaround is indeed now.
WHY NIGERIAN LEADERS PATRONISE FOREIGN HOSPITALS
It’s often claimed that the nation’s leaders abandon Nigerian hospitals because they refuse to fund them. This claim has gained popularity such that both the media and the general public cover up other anomalies that plague our hospitals. To begin with, I can confidently assert that I am a credible witness to problems affecting our hospitals since age 18, when I first landed in the hospital. I continued to patronise public hospitals till date. At a point when I had opportunities to attend private clinics, I instead continued to attend public health institutions. Even while abroad, anytime I visited Nigeria and needed to see a doctor, I still attended public hospitals. So, I am well informed about several factors militating against the smooth running of our hospitals.
Thus, I can confirm that our country is blessed with talented people in all fields of endeavours. Our public hospitals particularly parade many qualified hands that can perform feats comparable with their colleagues elsewhere. To buttress my point, I have been attended to by as many Nigerian doctors, nurses and pharmacists as possible in the UK. While I agree more funding is needed, as it is all over the world, other avoidable factors often overlooked are responsible for the poor state of our public health institutions. The factors are: poor maintenance culture, supervision and accountability gaps, care free attitude to work, corrupt practices, indiscipline to mention but a few. If the vault of the Central Bank is opened for our hospitals to take as much funds as needed, the above-mentioned factors would still militate against achieving results. The Management seriously need to focus on these areas. This is not the time to be in denial.
The bulk of donations for the deceased healthcare came from editors, journalists, notable families, and government functionaries. A retired general not only donated funds, but was at the hospital to check up on him, like many other figures. Mr Henry of the famous Ibru Organisations not only mobilised for funds, but was always at the hospital until his death. All these notable personalities were calling every day to get progress reports on his state of health. They are all now aware of credible reports that his death was avoidable had the medical personnel carried out their duties diligently. As the case of Ibrahim Kayode Sule has confirmed, like many others, those in government are aware of how people die in our hospitals owing to systemic medical negligence by the health workers. It thus follows that government officials who have lost family members and friends (like Ibrahim) in questionable circumstances, would not risk their own lives in the hands of the same medical personnel, but would rather use statutory public funds to go for healthcare abroad. The first law of nature is the preservation of one’s head. Anyone in a position of authority, either in public or private enterprise, would therefore not hesitate to take advantage of such opportunities for better medical care. The implications are that, the nation’s hospitals are losing vital revenues to foreign countries; while the nation’s medical personnel carry the tag of incompetence (though they’re qualified and competent to do the job).
Of course, I would not be surprised if those in charge of the deceased’s healthcare deny wrongdoings, but what matters is whether the Management will allow the damaging culture of medical negligence to thrive. I also hope that the Management realises the implications of avoidable deaths of patients under their care on the institution’s corporate image and survival. His death almost immediately reached the seat of power prompting the Senior Special Assistant to the President, Garba Sheu to make calls and commiserate with other colleagues over his death. The lesson from this episode is that, doctors and nurses need to cool down and begin to treat patients who come before them with dignity and respect no matter the patients’ background. A doctor’s fulfilment lies in upholding his/her Hippocratic Oath as a life saver, and not someone on a high horse looking at others as inconsequential and deserving less respect.
Ibrahim Kayode Sule is dead and buried, never to be seen again. But the question remains: how many more Nigerians will end up like him?
I thank the Chairman of the Medical Advisory Committee for his time in perusing my submissions.