In November 2021, Babagana Zulum, Borno governor, uncovered two primary health centres (PHC) in the state where officials were found to be extorting patients and collecting money for services and drugs that were meant to be free. A subsequent investigation undertaken by a team of reporters has revealed that the situation is not only prevalent in Borno, but in other states across the country. Findings showed that these unwholesome practices pose a cog in the wheel of Nigeria’s fight against malaria.
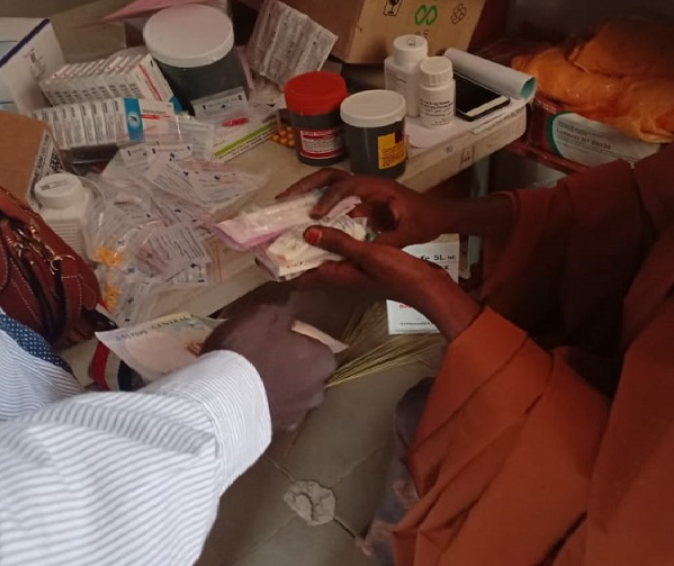
Fatmata Ahmed, 27, was downcast as she stood motionless at the entrance of Mairi PHC in Jere, a community in Borno state. The middle-aged lady had tested positive for malaria but was asked to bring money for drugs before she would be treated. The mother of two, who sells bean cake in the neighbourhood, was unable to afford the treatment.
“I just paid N500 for a malaria test. They are now asking me to bring another sum of N1,500 before they will give me drugs,” Fatmata lamented.
“I am a bean cake seller, even the total amount I made from today’s sale is not up to N1,000. I don’t know where they are expecting me to get N1,500.”
Advertisement

She left the clinic disappointed without getting the treatment needed to treat the illness she was battling.
Dispensing drugs without a diagnosis
The situation was the same at Dalaram PHC in Maiduguri, Borno state capital, where patients were asked to pay N200 for a malaria test.
Advertisement
The price for malaria drugs varied from N1000 upwards, depending on the drugs and injectables presented by the doctor on duty.
Aisha Musa, 35, was spotted sitting alone on a bench in the clinic, while other patients were seated closer to the entrance of the doctor’s room.
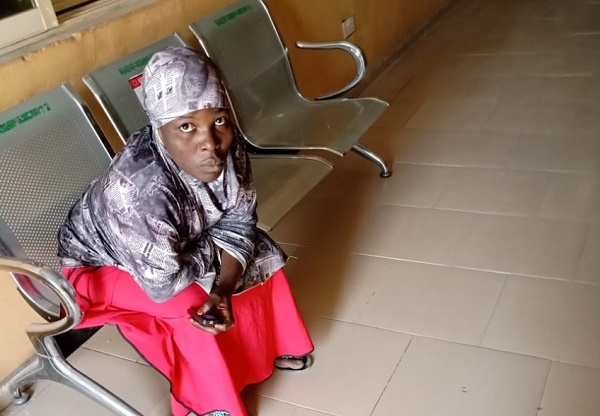
A reporter approached Aisha, who said she had just been diagnosed with malaria after paying N200. She said the doctor told her to pay another N1,000 for drugs.
“I am sitting here to call my husband who asked me to come here for treatment to inform him of the money they are asking me to pay. He will be the one to pay because I don’t have any money with me,” said Aisha.
Advertisement
The reporter later joined the queue and watched as the women entered one after the other, with many of them coming out looking befuddled.
After eventually entering the room, the reporter met three health officials and told them he had been battling a severe headache and loss of appetite.
“That’s malaria,” one of them retorted.
Without conducting any test on him, he was prescribed drugs and asked to make payment in the next room, where a woman identified as Sadia Bukar demanded N1,200 before handing over the drugs.
Advertisement
When contacted about why PHCs were charging patients for malaria drugs and tests, Juliana Bitrus, the Borno commissioner of health, refused to respond to text messages or pick up calls over several weeks.
Multi-million dollar fight against malaria
Malaria, a disease caused by the plasmodium parasite and transmitted by the bite of infected mosquitoes, kills hundreds of thousands of Nigerians annually.
Advertisement
According to the latest report by the World Health Organisation (WHO), there were an estimated 241 million malaria cases and 627,000 malaria deaths — mostly children under five — worldwide in 2020.
The UN agency noted that Nigeria accounted for around 27 percent of malaria deaths in the year under review.
Advertisement
Also, the WHO report estimated that 76 percent of Nigeria’s population is at risk of malaria by living in high transmission areas.
To curb the spread of the disease, the Nigerian government and its partners have committed millions of dollars to the fight against malaria.
Advertisement
These funds are being deployed for malaria prevention and treatment programmes, which include free antimalarial drugs and rapid diagnostic test (RDT) kits.
For instance, the federal government secured a $364 million credit facility from three multilateral banks; the World Bank, African Development Bank, and Islamic Development Bank to fund health sector interventions in 13 states for five years (2020–2024) against malaria.
Global Fund, an international organisation working towards ending AIDS, tuberculosis and malaria as epidemics, has also continued to fund the fight against malaria.
In March 2021, Global Fund launched three new grants to strengthen the fight against HIV, TB and malaria and build resilient and sustainable systems for health in Nigeria. The new grants, covering the 2021-2023 implementation period, are worth $900 million.
As a result of these programmes, anti-malaria drugs and RTD kits, are distributed in many states — including Kaduna, Kano, Katsina, Jigawa, Kwara, Niger, Taraba, Gombe, Yobe, Adamawa, Ogun, Osun and Delta.
PHCs under support ‘extorting’ patients in Kwara
On a monthly basis, some PHCs in Kwara state get free RTD kits and anti-malaria drugs expected to be dispensed without charge to patients. But this is not the reality on the ground.
At the Basic Health Centre in Ijagbo, Oyun LGA of Kwara, one of the beneficiaries of the scheme, the nurses insisted that they will run a malaria test on the reporter when he reported symptoms.
However, after the test was conducted, he was not told whether it was positive or negative. Instead, one of the female nurses, identified as Ajayi, asked for the bio-data of the reporter and penned down the information on a sheet of paper.
Minutes later, she brought out some drugs: artemether, paracetamol, albendazole, amoxicillin, B-complex and Folic acid. All of these, according to her, cost N1600.
To ascertain the cost of the anti-malaria drug and determine if the facility complies with the free dispensation of the drug, the reporter asked Ajayi to remove paracetamol and amoxicillin from the list.
Suspicious, Ajayi’s colleague got angry and withdrew the already dispensed drugs. The nurses asked the reporter to get them at a drug store when he claimed malaria drugs should be free. After both parties haggled for some time, the reporter eventually succumbed and paid N700 for the malaria drug.
The same scenario played out in Awoli PHC in Ilorin, another centre benefitting from free drug supplies.
The nurse on duty, after listening to the complaints of the reporter, demanded that he should get a registration card, which cost N300.
Afterwards, the female nurse led the reporter to a room dedicated to laboratory activities where the personnel on duty ran a rapid malaria test on him, and the results came out negative.
In spite of the test result, some drugs including paracetamol and an anti-malaria tablet were prescribed, costing the reporter N1,500.
‘Global Fund dropped one hundred PHCs for corruption’
Nageri Abdullahi, an official at the Kwara State Malaria Elimination Programme, confirmed that sharp practices were prevalent in primary healthcare centres.
“We are aware that some PHCs are engaging in such practices,” he said. “We are instigating the citizens to keep reporting those PHCs.”
Abdullahi said the health centres had also been directed to exempt malaria patients from the collection of cards.
He further explained that many PHCs that were previously benefitting from free drugs and test kits have been dropped over lack of accountability.
“We had 450 facilities that we were supporting before now. Out of these 450 facilities, many didn’t meet up. Even though the state was also supporting 80 facilities too. But they were unable to account for the supplies,” he said.
“For instance, If they claim that they tested 100 people in a month and seventy people tested positive, that means seventy anti-malaria drugs should be dispensed but their figures were not matching up. That’s why Global Found dropped over 100 facilities.”
In the presence of the reporter, Abdullahi put calls across to the local government officers in charge of the PHCs visited, cautioning them to desist from extorting patients.
He also threatened that the state will take a decisive step against those found culpable.
Osun insists malaria drugs are free — but we found the opposite
In Osun, Rafiu Isamotu, the commissioner for health, maintained that anti-malaria and HIV drugs were free at the general hospitals and PHCs across the state.
“Essential drugs are meant to be provided for free,” he said during a telephone interview. “We commissioned some pharmacists in the health facilities. They will bring the invoice of drugs given to patients at the end of the month, and we will pay them.
“They must be given free of charge after you have been tested or provide credible evidence that you have malaria.”

To put the commissioner’s assuredness to test, a reporter visited the Osun State General hospital alongside an associate, who feigned illness.
At the hospital, the associate approached a doctor to complain that he had malaria symptoms — and some drugs were recommended.
The doctor wrote four different antimalarial drugs on a piece of paper and directed him to the pharmacy.
Since the commissioner had earlier said antimalarial drugs were free, he confidently proceeded to the pharmacy but it was a different situation upon arrival, as the attendant insisted that N1,260 must be paid before the drugs would be provided.

Amid efforts to persuade the attendant that the drugs should be free, other patients without money were seen calling their loved ones to send money to get recommended drugs.
After making payment for the drugs, the pharmacy issued a receipt from Akol Pharmacy Limited, a company managing the hospital’s pharmacy.
Asked why the hospital’s pharmacy was handed over to a private firm to manage, the commissioner of health said “at some point when the state government had difficulties in paying salaries and could not provide drugs at general hospitals, we outsourced [to] some pharmaceutical companies because we do not want our hospitals to be without drugs.
“We asked the pharmacies to provide drugs in the hospitals at discount. But essential drugs like anti-malaria medicines are to be given out free to patients and at the end of the month, they will bring their bills to the government and we pay them. So, anti-malaria should be free.”
But it was not free — and Isamotu did not respond to enquiries asking if the state government was aware of the situation.
Efforts to speak with Akol Pharmacy Limited proved abortive, as the pharmacy did not respond to enquiries sent by our reporter.
‘Corrupt practices threatening anti-malaria fight’
Health experts say the sharp practices involved in the dispensing of drugs have contributed to the inability of the country to overcome malaria, despite sustained international support.
Franklin Owusu, a medical consultant, said such petty corruption must be curbed to sanitise the health sector.
Owusu said health-related corruption, which he said often comes in several forms like absenteeism of healthcare workers, extorting and stealing from patients, must be stopped if the goal is to move the sector forward.
“There is no way the country and the health sector can move forward if this petty corruption is not tackled,” he said.
He added that there is a need for the government to put in place necessary measures to end the practice.
Aisha Lawal, a public health practitioner, stated that dispensing drugs without proper medical tests is tantamount to self-medication, which she said poses a threat to combating diseases like malaria.
“When you indulge in getting drugs without a proper medical test, the person giving and the person receiving the drugs are doing a great disservice to themselves,” Lawal said.
“First, the medical doctor or pharmacist giving out the drug can have his licence seized if caught and the person at the receiving end could be exposed to incorrect choice of therapy, masking a severe disease and as well, putting himself at the risk of dependence and abuse.”
FG ‘turning a blind eye’
Debo Adeniran, chairman, Centre for Anti-corruption and Open Leadership (CACOL), says the government is looking the other way as corruption eats deep into the health sector.
He said the government has always been aware of the corrupt practices but refused to take decisive action.
“We expected that the government at all levels will ensure that all essential supplies made to the PHCs are properly utilised but sadly, this corruption has continued unabated for years,” he lamented.
Adeniran advised the government to set up sting operations and bodies that would serve as a task force to curb the corrupt practices.
“There is a need for the government to indulge in a more undercover investigation to arrest those who are perpetrating this act, get them arrested and prosecuted to serve as a deterrent,” he added.
Established in 1992, the National Primary Health Care Development Agency (NPHCDA) is saddled with providing a network of services, benefits, and resources to empower healthcare delivery in the country.
TheCable contacted the spokesperson of the agency, Sa’adu Salahu, who said: “We do not run hospitals. You should reach out to ministries of health.
“We [only] intervene to ensure that things work better. The PHCs are not under our control. I will advise you to direct your questions to the health ministries in the affected states. “
Olorunnimbe Mamora, the minister of state for health, also did not respond to calls and multiple enquiries sent via SMS.
The ministry’s spokesperson, Ahmadu Chidanya, after multiple calls, replied with an SMS, asking the reporter to bring questions on the matter to the next ministerial briefing at the state house.
He declined further comments on the matter.
Contributors: Alfred Olufemi, Niyi Oyedeji and Adejumo Kabir
This investigation was supported by the African Investigative Journalism Conference, the Gates Foundation and the Henry Nxumalo Foundation